Overview
This activity is designed to help middle school students understand the importance of physical activity in maintaining stable blood sugar levels. Through interactive learning, students will also be introduced to a variety of careers related to blood glucose management and diabetes care. These hands-on activities were developed by the COE Health in collaboration with the New Brunswick Community College (NBCC) to support health literacy and career exploration among youth.
NB Curricular Connections
Strand: Personal Wellness
Big Idea: Healthy Lifestyle
Grade 6- Examine their personal health habits and their impact on the seven domains of wellness.
Grade 7- Describe the impact of health habits on self and the community.
Grade 8- Evaluate the impact of health habits on self and community well-being.
Big Idea: Thinking About Potential Career Pathways
Grade 6- Critically investigate and describe the labour market and preferred career pathways.
Grade 7-Critically investigate and describe the labour market and preferred career pathways.
Grade 8-Critically investigate and describe the labour market and preferred career pathways.
Strand: Well-Being
Big Idea: Physical Fitness Concepts
Grade 6-Apply physical fitness concepts to construct personal wellness goals.
Grade 7-Apply personal wellness SMART goals that use fitness concepts.
Grade 8- Apply personal wellness SMART goals that use fitness concepts and principles.
Activity: How Exercise Helps Lower Blood Sugar
You’ll act out how sugar, insulin, and exercise work in the body — and see how exercise helps lower blood sugar, especially for people with type 2 diabetes.
What You’ll Need:
*All materials are included in PDF form*
- 5–7 signs that say “Glucose (Sugar)”
- 3–4 signs that say “Muscle Cell”
- 2 signs that say “Insulin”
- 1 sign that says “Type 2 Diabetes”
- 1 sign that says “Exercise”
- A short PDF or slideshow about type 2 diabetes and different careers that surround blood glucose and diabetes (for the teacher to explain first)
Step 1: Learn First!
Before we get active, your teacher will explain (Blood sugar in motion PDF attached):
- What is glucose (sugar)
- What does insulin do (helps sugar get into muscle cells)
- What happens in type 2 diabetes (insulin doesn’t work very well)
- How exercise helps the body use sugar
Step 2: Assign Roles
- 5–7 students will be sugar (glucose)
- 3–4 students will be muscle cells
- 2 students will be insulin
- 1 student will be exercise
Step 3: Act It Out!
Part 1 – No Exercise
- Sugar students stand beside muscle cell students.
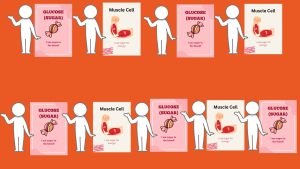
- Insulin students try to help sugar get inside the muscle cells (pretend to “unlock” doors of the muscle cell students).
- BUT… insulin can only open 2 of the doors.

- Only 2 sugar students get inside (2 sugar students stand behind muscle cell students).
- The rest stay “stuck” in the blood (pretend to float around the room).

“This is what happens in type 2 diabetes. The body has insulin, but it doesn’t work very well. More sugar stays in the blood.”
Part 2 – With Exercise
- Everyone does a little bit of real exercise! (jumping jacks, push-ups, dancing!)
- Sugar students stand beside muscle cell students.

- The exercise student goes around and “opens” all the muscle cell doors.
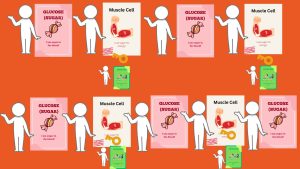
- All the sugar students go into the muscle cells (all sugar students stand behind muscle cell students)!
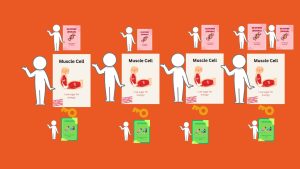
“Exercise helps open the doors even without insulin! So sugar leaves the blood and goes into the muscles to be used for energy.”
Step 4 – Let’s explore the roles of professionals who work with blood and Diabetes
- First contact:
If you are experiencing mild to moderate symptoms of high blood sugar such as, feeling very thirsty, frequent urination, blurry vision, headaches or fatigue it is important to proceed to your family doctor, nurse practitioner or a walk in clinic.
If you are experiencing severe symptoms of high blood sugar such as, extreme thirst and dehydration, rapid breathing or fruity-smelling breath, confusion or drowsiness, nausea and vomiting or loss of consciousness you must go to the emergency room or call 911.
Once you have had the initial conversation with a doctor or nurse practitioner, getting a referral to a dietician and to the diabetes education center is important for ongoing treatment.
The Fredericton Diabetes Resource Centre offers services for children and adults living with type 1 diabetes, type 2 diabetes, gestational diabetes, and prediabetes, with Registered Dietitians, Nurses, Social Workers, Podiatrists and Pharmacists on staff. The types of services provided are pediatric diabetes clinic, classes for newly diagnosed diabetes and pre-diabetes, insulin and medication adjustment, diabetes education and support (lifestyle, diet), high-risk diabetes foot clinic, and smoking cessation counselling.
- Medical Laboratory Technologist: Medical Laboratory Technologists are responsible for specific lab tests that are essential for diagnosing diabetes before regular monitoring, dietary support, and other interventions begin. There are also ongoing lab tests that complement glucometer checks (such as HbA1c and kidney function evaluations) which are important for long-term management.
- Doctor: The doctor decides how often blood glucose should be monitored—this may range from once daily, to before every meal and at bedtime. The doctor also prescribes the amount of Insulin or oral medication a patient may need depending on their blood sugar levels.
- Patient Care Attendant/Personal Support Designation or Nurse: Depending on the hospital and unit of the hospital, Registered Nurses (RNs), Licensed Practical Nurses (LPNs) or Patient Care Attendants are responsible for checking blood sugar levels. For example, if a Doctor orders blood sugar checks four times daily (before each meal and at bedtime), the nurse or PCA will perform these using a glucometer. This involves cleaning the finger, pricking it with a lancet, and applying the drop of blood to a test strip.
- Nurse: If the patient’s blood sugar is elevated, the nurse checks the doctor’s insulin or oral medication orders, to determine if either is needed and how much. The nurse then administers the appropriate dose. PCAs cannot administer insulin or oral medications. The nurse also documents the blood sugar level and communicates with the healthcare team as needed to ensure the patient’s blood sugar remains within a safe range.
(See medical map for visual of professionals who work with diabetes!)
Extension ideas (optional)
Please see attached the experiential learning extension student worksheet:
Students will research and explore a medical career pathway of their choice, then share their findings in an interactive and creative format to deepen their understanding of healthcare roles.
Extension Activity
Discuss with the person sitting next to you, your favorite type of physical activity that could be incorporated into your everyday life, to help keep blood sugar levels stable (Biking, walking, running, swimming, sports).
Discuss what changed with the blood sugar between the activity with exercise and with no exercise.
Reflection Activity
Please see the attached PDF for several choices on how you and your learners can reflect upon today’s activity.
Global Competencies
Resources
- American Diabetes Association. (n.d.). Understanding blood glucose and exercise. https://diabetes.org/healthy-living/fitness
- Cleveland Clinic. (n.d.). Insulin: What it is, what it does, how to take it & side effects. Cleveland Clinic. https://my.clevelandclinic.org/health/treatments/22769-insulin
- Mayo Clinic. (n.d.). Type 2 diabetes – Symptoms and causes. Mayo Foundation for Medical Education and Research. https://www.mayoclinic.org/diseases-conditions/type-2-diabetes/symptoms-causes/syc-20351193




